How To Evaluate a Restricted Lingual Frenum: A Guide to Help You Understand the Complexity of a Tongue-Tie Diagnosis and the Importance of Evaluating the Whole Person For Myofunctional Impairment
Why a Tongue-Tie Diagnosis Matters
Tongue-tie diagnosis has come a long way since many practitioners were trained. There are a few different methods for tongue-tie diagnosis. It is multifaceted and the reasons for identification have moved beyond articulation concerns or difficulty licking an ice cream cone.
An experienced orofacial myofunctional therapist (OMT) will help evaluate you as a whole. The big picture of myofunctional impairment is more important than just the tie itself.
In my practice, I use an adaptation from the Lingual Frenulum Protocol (Marchesan, 2014) for my screening of the lingual frenum.
I look at 3 general tests. The difference in mouth opening with and without tongue tip to the incisive papilla (not suctioned), alterations to the shape of the tongue during elevation, and the frenulum fixation.
I then look at several functional tests (like tongue mobility, tongue protrusion, and tongue lateralization) and evaluate how you feel when moving your tongue through those motions.
Failure to get an accurate tongue-tie diagnosis can lead to a lifetime of problems.
Who Can Diagnose a Tongue-Tie?
There are several professionals that can complete a tongue-tie diagnosis, but the question is…is it being done? Depending upon where the doctor or professional was trained, he or she may not understand the complexity of a tongue-tie, or he or she may not even believe that a tie is a concern. Herein, lies the problem. Again, this is why I encourage my audience to go right to the professional who knows, an experienced myofunctional therapist so that nothing gets overlooked.
Can a Tongue-Tie Affect Speech?
Yes, a tongue-tie can create speech challenges, some of which are never really thought about. Two of the most common things that I hear from parents is:
- My child has been in speech therapy for a long time and never makes any progress
- My doctor says my child has a tongue-tie but it doesn’t matter unless it is affecting the speech or hurts to lick an ice cream cone
This couldn’t be further from the truth, and it is an unfortunate part of my job as an educator. Many children have trouble with articulation or speech mechanics, and very few ever lift and look under the tongue. My own granddaughter suffered through 3 years of unsuccessful speech therapy. Once I made a tongue-tie diagnosis and implemented therapy she made large strides in her speech therapy.
Common red flags for a tongue-tie are trouble with certain sounds (like T, D, L, N, and R), delay in speech development, or having a lisp. There are others, but these are the most common in my practice.
What Are Tongue-Tie Symptoms and Signs?
- Difficulty lifting the tongue or moving it sideways
- Inability to stick tongue out
- Tongue that appears notched, tethered or heart-shaped when sticking it out
- Difficulty or inability to breastfeed
- History of colic, gassiness, spitting up, acid reflux or latching issues as an infant
- Speech challenges
- Swallowing / chewing difficulty
- Tongue resting in the floor of the mouth
What Does a Tongue-Tie Look Like?
I get asked this question a lot and this is why a comprehensive myofunctional evaluation matters.
This tethered oral tissue is just a piece of a much bigger puzzle. A tongue-tie might look very obvious when attempting to lift the tongue. I call this “low hanging fruit” because it is easy to identify. But, what about the tongue-tie diagnosis when it is not low hanging fruit? There could possibly be a deep, posterior tie, or a mild-moderate restriction that will only catch the eye of a trained and knowledgeable OMT.
When you have a comprehensive myofunctional evaluation, I look at much more than just the frenum. I look at:
- Medical History
- Allergies
- Childhood History
- Past and Present Airway & Breathing Concerns
- Speech History
- Sleep Apnea / Snoring Concerns
- Digestive Symptoms
- Swallowing
- Chronic Head and Neck Tension
- Facial Structure Evaluation
- Mouth Resting Posture
- Tongue Posture
- And more…..
During your evaluation, I will help you understand your myofunctional impairment and why you have the symptoms you do. I use this evaluation, to not only educate you but to help me create the best therapy plan for you!
How To Grade a Tongue-Tie?
Using two measurements, I calculate the TRMR (Tongue Range of Motion Ratio).
Grade 1: TRMR > 80%
Grade 2: TRMR 50-80%
Grade 3: TRMR 50-25%
Grade 4: TRMR < 25%
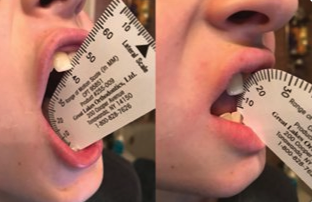
Some ties are very obvious, and others are identified as”mild” but still require a frenectomy due to all the myofunctional impairment present. A Grade 3 or 4 tongue-tie is normally the biggest concern, in the eyes of the practitioner, BUT not in the eyes of an OMT!
The general rule of thumb is that anyone who has a TRMR less than 50% needs a frenectomy. However, I have had many clients with a better ratio, still, require a frenectomy based upon the rest of their myofunctional impairment snapshot.

About Carmen
Carmen found her path of passion years ago as a dental hygienist. After a stint in graduate school to earn her M.B.A., she left clinical hygiene practice to start her business, Integrative Myofunctional Therapy. In addition to seeing clients in her private online practice, she also teaches the craft of myofunctional therapy in her Myo Mastery Program, coaches dental offices on how to implement myofunctional screening into the daily practice, and speaks frequently in various settings.
Carmen is a provider for the Foundation of Airway Health, where she works diligently for the recognition, diagnosis, and treatment of airway related disorders.
In addition, she is a proud member of several professional associations that afford her the opportunity to learn so that she can help her clients. Her professional memberships include:


